What is tendinopathy?
Pain, swelling and impaired performance of a tendon.
It is now widely encouraged to use the term ‘tendinopathy’ instead of the outdated ‘tendinitis’. Tendinopathy describes a constellation of symptoms involved in this condition. This term does not indicate any structural change happens on the tendon.
The term ‘tendinitis’ still being used on lots of web pages, and you may even see in some medical reports. Tendinitis is inaccurate. ‘itis’ means something that is inflamed. Though there are some inflammatory changes observed in a painful tendon, and inflammation is our body’s repair process, the exact role of inflammation in tendinopathy is still unclear.
Lets understand what happens in tendinopathy..
Researchers use experimental and clinical studies to understand how and what might happen in tendinopathy as it is not entirely possible to mimic real-world day-to-day scenarios on a living structure like a tendon. There are two popular understandings exist in the tendinopathy world.
The continuum model
Central nervous system model
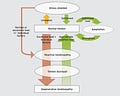
The continuum model of tendinopathy was first proposed in 2009 and later updated in 2016 by Jill Cook and Craig Purdam. This continuum model proposes 3 stages in the life of a painful tendon.
Reactive
Disrepair
Degenerative
When the load/ activity exceeds the capacity of a normal tendon, either suddenly or within a short period, it creates a reaction on the tendon. This would result in pain, limitation of movements, and some obvious thickening over the site of the tendon – this is reactive tendinopathy. This is a non-inflammatory response of the tendon to the load.
This can be understood by an example: if you have never exercised regularly and suddenly you decided to go for a long run or decided to clean your windows. Following this sudden increase in activity, sometimes you may develop pain in a specific site or during a specific action.
When this irritable load is removed and if sufficient healing time is available for the tendon, it then resumes to its pre-reactive stage; where pain may settle within few weeks but sometimes the swelling over the site may take longer to settle or never will. This isn’t abnormal, the tendon would have thickened inside. This is an adaptive response.
However, if the load/ activity persists or if there is not enough healing time, then the tendon goes through to the next stage which is disrepair (repeatedly overloaded tendon).
An example would be, once the pain is settled, instead of doing a short gradual return to the activity, if the person gets back straight to the same amount of running as he/she did on the first episode, then this will set off a further reaction on the tendon. In this stage, pain and stiffness could persists for longer duration after activity, or sometimes even at rest also can be painful at night times affecting sleep.
If there is a continued state of these above unfavorable environment – ie. repetitive overload, insufficient rest, combined with other comorbidity like diabetes, vascular problems, smoking history, then the tendon goes to degenerative stage, here the tendon may not repair, sometimes even result in rupture.
The short coming of this model is that this is insufficient to explain all types of tendon pain. Because this model is mainly based on structure and loading abnormality. Sometimes even exact training parameters, strengthening exercises and recovery periods are followed, some tendon pain would not improve. In other cases, there may not be any evidence of repetitive loading or any activity related injury and a person would still develop tendon pain. So this model lacks all possible explanation for tendon pain.
Model 2:
Another model to understand tendinopathy is the central nervous system. Our central nervous system (includes the brain, spinal cord, and all nerves in our body) is continuously sampling all our tissues in the body via the nerves - the state of the tissues, their capacity, and their energy reserves are continually relayed to the brain by our nerves. When there is any deficiency in the muscle capacity or any potential threat of damage, the brain creates a painful experience for that person, so the person would look after the body site that needs attention.
Increasing amounts of research points out that a structural model like the continuum model is insufficient to answer all possible explanation therefore it is essential to take the central nervous system model along with the local structure model in the management of tendinopathy.
Relationship between structure, pain, and function
Tendon pain can be debilitating. Research shows that the nerve supply to the actual tendon itself is limited. And often tendon pain can be spotted precisely but you may also experience pain that can spread over an area - a hyperalgesia response from tendon pain. How does this happen when there is a very limited nerve supply?
The tendon pain remains a mystery.
It could be cell-to-cell signaling process via chemicals, – ie. Cells in tendon will inform the nearby receptors ( Mechanoreceptors) and thereby nociception (here nociception means information, not pain) is conveyed to the brain- and the brain will decide whether it should produce pain on the site. It all happens in split seconds.
Secondly, US scan or an MRI done in tendinopathy would reveal disorganization in cells and its network in the tendon ( called the matrix), will show presence of fibrin in tendons, there would be increased blood vessels, and changes in tendon cell sizes. These changes were once believed as a pathology/ source of pain.
However it is not sure whether the inflammatory changes observed in a painful tendon are similar to those inflammatory changes around a injured/wounded tissue. Furthermore, it is interesting to note that, asymptomatic tendons also show similar changes like a painful tendon presents under the scans like Ultrasound or an MRI. So we don’t know whether inflammation is the primary cause of pain and its relevance in tendon pain.
A large body of research recommended specific way of loading exercises to reorganize those structural changes and expecting that it would to improve tendon pain. But current evidence informs that those structural changes does not always correlate with tendon pain.
In addition to that, most electrotherapeutic modalities like therapeutic ultrasound or shockwave are proposed to reduce inflammation. Whilst there are inflammatory processes in tendon pain, those cannot be our treatment targets. When the true mechanism involved in tendinopathy is unclear, management of inflammation alone may not result in a successful treatment outcome and obviously, won't help the patient.
Tendon pain is not merely an inflammatory process, and not just a structural problem. It is multifactorial – a combination of biochemical, structural changes, cell signaling changes and central mechanisms.
This takes us next to how to manage this complex tendon pain??
What we observe in the real world is that the tendon pain can take a long time to improve.
Electrotherapy modalities appear to offer pain relief, but often will improve pain for a short term, meaning- some pain relief between few days to a few weeks and symptoms resume. Also, these modalities won't change the pain processes involved in tendinopathy, which is a complex process, remember not just inflammation.
As we have seen above that the structure of the tendon itself has limited or in most cases no contribution to pain, it is futile to target the tendon structure alone for pain relief. What I mean by this is- the treatment interventions such as taping the tendon, friction massage over the tendon, needling techniques, and other electrotherapeutic modality over the actual tendon carry no meaningful long-term benefits.
Loading the tendon- which is exercises has the best quality evidence in the management of tendinopathy.
The recommended strategy is to gradually load the muscle/tendon/ joint with relative rest periods and improve the overall capacity of the individual so that our functions can be made more manageable.
Explaining people what happens in the tendon ( only if needed) can also reassure them to engage in the exercise program. Often people would be worried that in case they may rupture the tendon by doing their normal activities or exercises. Also they want to know what works quickly ( for all the valid reasons, its not nice to be in pain). But there are no shortcuts in the management of tendinopathy, injections like corticosteroids are not safe on the tendons.
So, what type of exercise?
Conventionally, there are a few types of exercises that were used in the management of tendinopathy. Most popular one is eccentric type of exercise. And there are concentric and heavy slow resistance types of exercises.
To be honest, as much as we know that exercises are the best in the management of tendinopathy, we don’t know what type of exercise, how many sets and reps, and how often a week should be done- these dosing parameters are unclear.
But you may be reassured to know that all type of exercises works in its own way.
The parameters vary between the patient group. For example, I would plan the program for a patient depending on their age, daily functional needs, work status, and recreational activities. There is no standard exercise recipe for Achilles tendinopathy, the program must be tailored to suit the individual needs. You may use SIN factors (severity, irritability and nature) to guide your choice of exercises at early stage of rehabilitation.
Finally, it is vital to progress the exercise depending on patient goals.
So the take home message is, that the main problem is never just the tendon.
Load the tendon
Progress the load
Tailor the loading program to suit patient’s needs
If you have come this far, thank you and see you next time in another post.
Cook, J. L., & Purdam, C. R. (2009). Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. British journal of sports medicine, 43(6), 409–416. https://doi.org/10.1136/bjsm.2008.051193
Littlewood, C., Malliaras, P., Bateman, M., Stace, R., May, S., & Walters, S. (2013). The central nervous system--an additional consideration in 'rotator cuff tendinopathy' and a potential basis for understanding response to loaded therapeutic exercise. Manual therapy, 18(6), 468–472. https://doi.org/10.1016/j.math.2013.07.005
Cook, J. L., & Docking, S. I. (2015). "Rehabilitation will increase the 'capacity' of your …insert musculoskeletal tissue here…." Defining 'tissue capacity': a core concept for clinicians. British journal of sports medicine, 49(23), 1484–1485. https://doi.org/10.1136/bjsports-2015-094849
Rio, E., Moseley, L., Purdam, C., Samiric, T., Kidgell, D., Pearce, A. J., Jaberzadeh, S., & Cook, J. (2014). The pain of tendinopathy: physiological or pathophysiological?. Sports medicine (Auckland, N.Z.), 44(1), 9–23. https://doi.org/10.1007/s40279-013-0096-z
Cook, J. L., Rio, E., Purdam, C. R., & Docking, S. I. (2016). Revisiting the continuum model of tendon pathology: what is its merit in clinical practice and research?. British journal of sports medicine, 50(19), 1187–1191. https://doi.org/10.1136/bjsports-2015-095422
Couppé, C., Svensson, R. B., Silbernagel, K. G., Langberg, H., & Magnusson, S. P. (2015). Eccentric or Concentric Exercises for the Treatment of Tendinopathies?. The Journal of orthopaedic and sports physical therapy, 45(11), 853–863. https://doi.org/10.2519/jospt.2015.5910






The examples sounds very familiar 🤔 (perhaps someone in the family?) LOL!
Good post. Its really a complex matter. Best to leave to the judgement of therapist and, then work together to achieve the goals. (Perhaps trying to "understand it all " is not going to help the patient!)
Thank you.